
HOW TO BEST PREPARE YOUR CHILD WITH ASTHMA OR ALLERGIES FOR SCHOOL
It’s that time of year again! Summer vacation is over and the kids are getting ready to go back to school. This Summer may have been met with some allergy challenges because it has been one of the hottest Summers on record. You may be worried about how your child with allergies and asthma may fare during the school year. Well, here are my five top tips to get your child with asthma or allergies ready for the school year.
1) Make sure the school is prepared to take care of your child in case of an emergency.
This is important for all children but specifically for children with food allergy and asthma. Children with food allergy must always have an adult ready to administer an epinephrine injector, and children with asthma must have access to an albuterol inhaler. Older children and high school children may know how to administer their medication. However, depending on the school’s policy and what is allowed, they may be restricted to seeing the school nurse or having the teacher administer the medications needed. It is important to feel comfortable with the school’s plan of action in case your child’s condition is to worsen. Have you discussed the signs and symptoms of when your child may be having a food allergy reaction or asthma attack with their teachers or school nurse? Does the school provide this type of training to their staff? These are all important questions to find out. If not, find out if there are plans to do so. Remember, it only takes one person to start change.
2) Has your child recently been evaluated by their Allergist.
An updated visit to your child’s allergist is always important, even with the most stable conditions. If your child is following up with their Allergist as directed, then you probably don’t have anything to worry about. If it has been a year or more, it is important that you schedule a follow-up soon. Over a year, many things can change. Your child’s medical condition or medical needs may have changed. Your child is growing and weight changes may require a change in dosing. Also, you can find out if new medications or treatments may be available. In addition, refills on expired medications may be needed. Lastly, an updated action plan on how to treat your child’s condition may be needed.
3) Address how medications will be given
Going back to school may mean a new schedule for your child and possibly yourself. Most allergy and asthma medications are given no more than twice a day. However, it can be difficult to coordinate the administration of a mid-day or late afternoon medication. Working with the school and your Allergist to figure out the best plan to have your child’s medication delivered correctly and timely with little interference to their day can be achieved.
In addition, a teenage child who has been given the responsibility of taking their own medications may need to be checked on periodically. It’s not unusual for me to see a teenager with exacerbated symptoms, all because they forgot a few too many times to take their medication and an upset parent sitting by their side. If you find that your child’s symptoms seem to be worsening or if you are not refilling their meds as expected, you may want to check on if they are taking their medications.
4)Address how your child’s condition may be affected by extracurricular and sports activity
A child with asthma and/or allergies may need special attention when it comes to them playing a sport or participating in extracurricular activities. Will they play outside but they have a severe pollen allergy? Will their asthma symptoms start once they start running? Or do you think your child’s care may need to be optimized so they can do their best? These are all questions that may be playing in your head. Addressing your concerns with your allergist is the first step. There are many ways to keep your child’s symptoms under control, including pretreating with medications prior to activities.
Furthermore, Extracurricular activities such as pottery making, painting, cooking, horticulture, etc, may have your child contacting possible allergens that may need to be addressed. If your child finds themselves with hives or a rash after an activity, testing and avoidance may be warranted.
5)Discuss your child’s care with caregivers
Coordinating your child’s supervision and safety to and from school may cause for other people to care for your child. Whether it is a friend’s mom carpooling the children to school, tutors, babysitters or nannies, it is important that all caregivers are aware of your child’s medical condition and have a plan of action. If you don’t have a plan of action, one may be obtained by your Allergist. Having one in place, may be particularly important in small children who may have difficulty expressing what they are feeling. Discussing the plan of action with your child’s caregiver will also help to give you insight on how comfortable your child’s caretaker is in implementing the action plan. If your child’s caregiver is not comfortable in recognizing signs and symptoms of your child’s medical problem or not comfortable in administering emergent medication, then secondary measures may need to be put in place, such as pre-prepared foods in a child with food allergy to decrease the likelihood of an accidental exposure, or maybe even a new caregiver. Most importantly, they should know how to contact you in case of an emergency.

Out of the mouths of babes. This rockstar teen is using her voice for change!
This article, written by Lindsey Holt, rheumatologist Dr. Melissa Hawkins-Holt's teenage daughter, right before Thanksgiving, was shared widely and has made the rounds on Instagram, being shared over 400 times.
Her local Board of Education student representative read what Lindsey wrote and brought it up at a meeting.
Calorie tracking now no longer allowed in any county Health curriculum!!!!!! All high schools and middle schools in her home county are being notified immediately of the change.
#teenager #teen #girl #teenagers #cute #baby #teens #teengirl #teenagerposts #teenmodel #follow #timetobe #beautiful #instagram #instagood #bambina #bhfyp
#eatingdisorders #mentalhealth #anorexia #eatingdisorderrecovery #edrecovery #recovery #anxiety #depression #bulimia #eatingdisorder #selflove #selfcare #mentalillness #mentalhealthawareness #ed #anorexiarecovery #ocd #recoveryispossible #bingeeating #haes #mentalhealthmatters #ptsd #eatingdisorderawareness #ana #bulimiarecovery #selfacceptance #edfighter #edwarriors #bingeeatingdisorder
(https://www.physicianoutlook.com/articles/give-thanks-eat-what-you-want



Remembering my dear #mentor and #friend, Dr. Richard E. Fitzpatrick, well-renowned for his pioneering of many cosmetic dermatologic procedures, including #Laser #Skin #Resurfacing. But his greatest legacy truly was setting an example for us to follow of the virtues of a good physician: medical curiosity, compassion and humbleness.
(With my friends and colleagues, #CoolSculpting Specialists Carla Homez and Maria Ferrer.) #ASLMS 2014



NOVEMBER is MEN's Health Awareness Month!!! Join US on OUR MONTH LONG and LIFE LONG Journey to IMPROVE the QUALITY of MEN's HEALTH!!!
At YOU & WEE, YOU are OUR #1 and Wee are here to serve YOU!!!
Like, Follow, Subscribe and Share Our Posts to help educate yourself and provide Value to You and Yours!!
#ErectileDysfunction #benignprostatehypertrophy #Arcadia #Peyronies #EnalrgedProstate #diabetescare #penileprosthesis #penileimplant #lowerurinarytractsymptoms #urology #hormonereplacement #surgeons #medicine #menshealth #sexualhealth #physician #naples #treatment #qualityoflife #venice #tampa #orlando #sarasota #centralflorida #siestakey #thevillagesfl #saintpetersburg #prostatecancer #impotence #movember


Pediatricians and Pediatric Allergists play a fundamental role in health coaching of children with asthma. Children love and respect their pediatricians, and the majority of times will follow their doctor’s advice. In the case of asthma, this can lead to the successful management of acute episodes and overall improved health and quality of life.



Heart Disease is the Number 1 Cause of Death for Women in the United States, killing almost 300,000 women in 2017. In order to decrease your risk of Heart Disease, please follow these general recommendations:
* Exercise 30 min daily at least 3 days/week
* Eat a healthy, balanced diet, low in fat and processed foods
* Avoid drinking excess alcohol
* Stop cigarette smoking
* Manage stress by practicing Coping Techniques


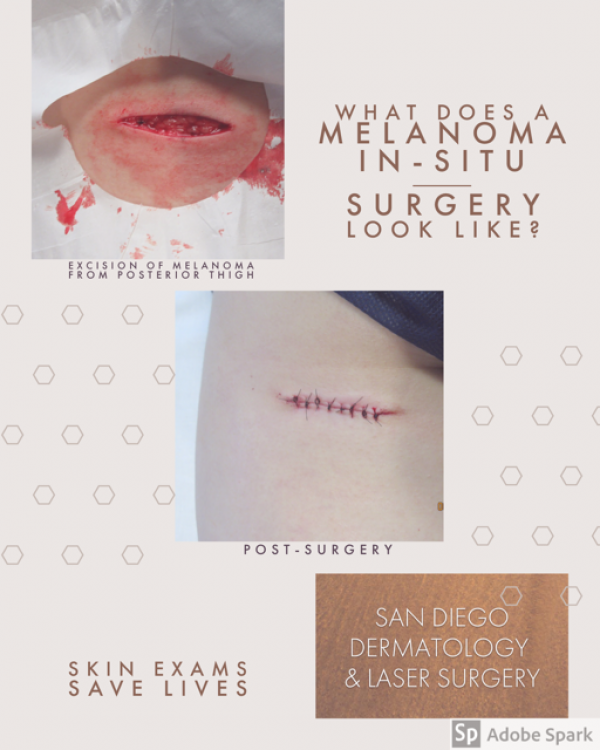
The key to a good MM prognosis-- EARLY DETECTION! Make sure to see your derm for routine skin checks, and follow up sooner if you notice any change in size, shape, color, itching and/or bleeding
This is great advice and guidance for all parents of school-age children. Thank you for sharing this information!